We study the immune response to transplanted organs in order to improve transplantation as a therapy.
Our lab has four main areas of investigation (1) costimulation blockade and costimulation independent rejection (2) xenotransplantation (3) transplant diagnostics (4) transplant outcomes.

As a transplant surgeon and scientist, Dr. Adams is interested in developing the best therapies and diagnostics for transplant patients, by understanding the fundamental mechanisms of the immune system that give rise to organ rejection. As a graduate student, under the direction of Drs. Chris Larsen and Tom Pearson, Dr. Adams investigated the efficacy of costimulation blockade, and helped develop Belatacept, now a clinically available therapy for transplant patients. Belatacept leads to improved survival and kidney function for renal transplant patients.
We are located at the University of Minnesota, Twin Cities, in the Diehl Hall building. Our lab is connected to the University of Minnesota Health Centre, and is composed of graduate students, post-doctoral research fellows, technicians and undergraduate students. We have active mouse, non-human primate, and clinical projects. Our research extends from basic science to transplant outcomes. We are a collaborative group, with active projects with researchers both at our home institution (the University of Minnesota), Emory, Georgia Tech and across the US.
Current Projects
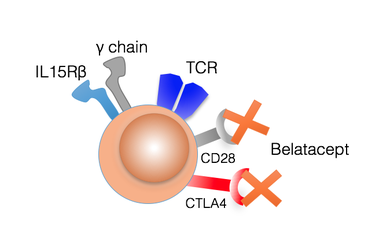
Costimulation Independent Rejection:
Our lab played a key role in helping develop a new approach to transplant immunosuppression. Instead of giving patients drugs which have effects on almost all the cells in your body, we developed an approach that specifically targets the cells responsible for rejection. This more targeted approach has led to improved survival and kidney function for patients. We have observed that there is still a set of patients that experience rejection despite this therapy, and our current aim is to understand this "costimulation independent" rejection, and develop targeted therapies that prevent rejection altogether.
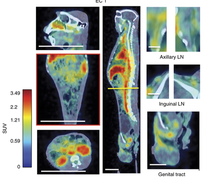
Transplant Diagnostics:
Transplanted organs are precious gifts. Organ rejection is a serious risk, and today, we are only able to diagnose rejection after it has already hurt the transplanted organ. Our lab is creating approaches, in collaboration with investigators at Georgia Tech, to detect rejection early, before it happens. We are creating a platform to detect rejection that patients can take home, and use weekly, so that every patient with a transplanted organ can monitor the health of their organ from home.
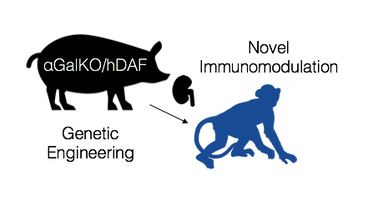
Xenotransplantation:
Everyone who needs an organ transplant today, does not receive an organ transplant. This means people are on an ever growing waiting list for life-saving organs, and everyday people die on that waiting list. Our lab is building on recent advances in genetic engineering and improved immunosuppression to create a scalable source of readily available organs for everyone on the waiting list. Our approach involves genetically engineering pigs and understanding the immune response to pig organs. We have had landmark success, with the longest recorded pig-to-primate xenotransplantation in history.
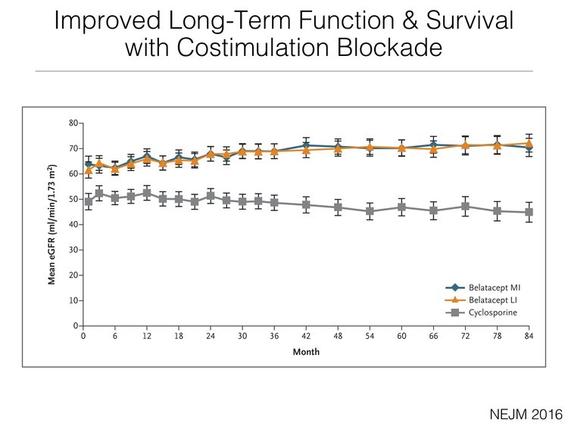
Transplant Outcomes
Transplantation is a team effort. Patients, families, donors, nurses, physicians, caregivers, scientists and surgeons all participate in the miracle of organ transplantation. We believe there is a responsibility to carefully measure how we are doing, and how we can do better. We carefully monitor how all patients treated at our center are doing, and use real-time data analytics tools to continue to improve our transplant outcomes, so patients live longer, healthier, happier lives.